Written by Amrit Tiwana & Sofia Bartlett
New research highlights important gaps, and promising opportunities, to improve sexually transmitted and bloodborne infection testing for people who use substances at harm reduction sites across British Columbia.
Sexually transmitted and bloodborne infections (STBBIs), including HIV, hepatitis C virus, and infectious syphilis, continue to be a major public health concern in Canada. These infections can have serious long-term health impacts if they are not diagnosed and treated early. At the same time, substance use has been increasing both globally and in Canada, which has contributed to rising potential for STBBI transmission among people who use substances. This makes timely access to STBBI testing and care especially important.
Testing is a critical first step. It helps people learn their status, begin treatment sooner, and reduce further spread. Yet many people still face barriers to testing, including people who use substances.
Why this research matters
People who use substances experience a much higher burden of STBBIs compared to the overall population. For example, in British Columbia, 45% of people diagnosed with hepatitis C in 2015 were people who use substances, despite representing a much smaller proportion of the overall population. Similarly, in Alberta, 42% of people diagnosed with infectious syphilis in 2022 reported using unregulated stimulants. While sharing drugs and drug-use equipment is the main route of transmission for STBBIs such as hepatitis C, the burden of infection among people who use substances is driven by wider social and structural factors. These include:
- limited or inadequate access to healthcare and harm reduction services,
- stigma and discrimination in healthcare settings,
- unstable housing, and complex health and social needs.
Together, these barriers make it harder for people to access STBBI prevention, testing, and treatment. Harm reduction sites, such as overdose prevention sites, supervised consumption services, and community-based programs, are often trusted, low-barrier spaces where people can access care.
This raises an important question: Are harm reduction clients able to access STBBI testing?
What we found:
We used data from the 2023 BC Harm Reduction Client Survey, which included 433 people accessing services across 23 sites in British Columbia (Figure 1), for this study.
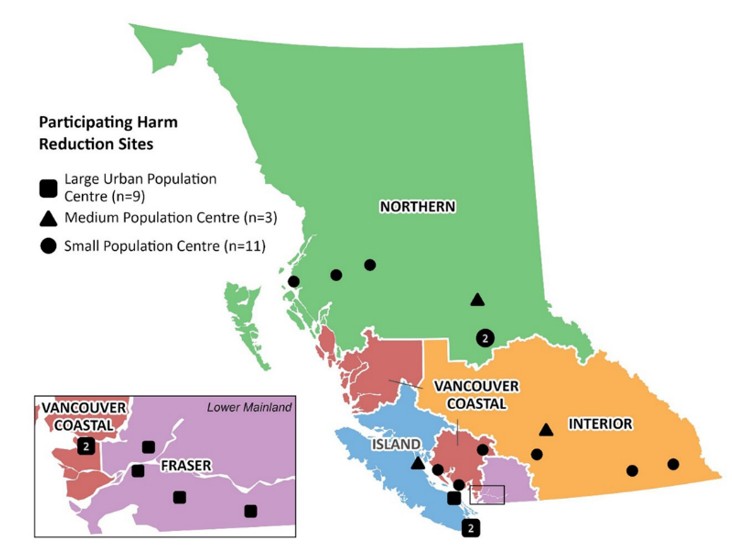
Figure 1. Map of participating harm reduction supply distribution sites in the 2023 Harm Reduction Client Survey in British Columbia, Canada. Available from the BC Centre for Disease Control.
Our study found important gaps in STBBI testing among survey participants, including:
- 38% of participants had not been tested for an STBBI in the past year
- Testing was lower among people in smaller communities
- Testing was lower in all other health regions compared to Vancouver Coastal Health
- Women were less likely to report recent testing compared to men
- Individuals receiving prescribed safer supply alternatives were more likely to have been tested
- Among participants who had been tested, nearly 1 in 4 did not know their test results
- 73% expressed interest in self-testing kits available through harm reduction sites
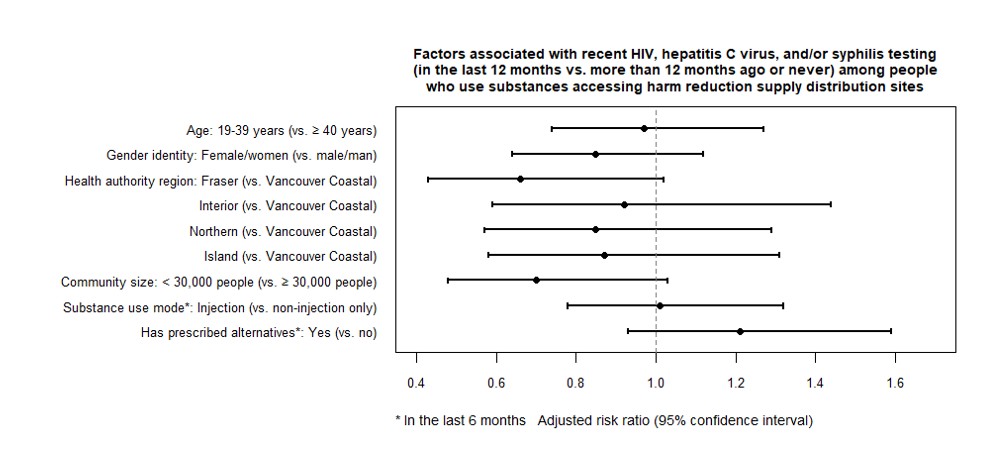
Figure 2. Factors associated with whether someone had been tested for STBBI in the past year compared to over a year ago or never tested.
While harm reduction sites in British Columbia reach many people and continue to be a critical component of STBBI prevention efforts, our study highlights that there are substantial gaps in access to STBBI testing among people accessing these essential services. Of note, we found that access to STBBI testing among people utilising harm reduction services is not equal across the province. People living in rural or smaller communities who access harm reduction services reported lower uptake of STBBI testing.
The role of harm reduction
Harm reduction services are uniquely positioned to support STBBI testing because they:
- Provide low-barrier, community-based care
- Are often trusted spaces for people who may avoid or not be able to access mainstream healthcare services
- Already offer services like naloxone, safer use supplies, and drug checking
By offering or facilitating access to STBBI testing in harm reduction services, people who are most impacted by STBBIs have more access to testing and care. Additionally, peer workers in harm reduction settings report high levels of satisfaction and personal benefit from providing STBBI testing and linkage to care, often experiencing improved confidence, job satisfaction, and mental wellbeing.
A promising solution: self-testing and self-collection
One of the most important findings from this study is the strong interest in accessing STBBI self-collection or self-testing through harm reduction services. Dried blood spots (DBS) are a type of specimen that can be used for STBBI testing. Finger-prick blood is used for DBS specimens, which can be safely self-collected. Offering self-collection of DBS for STBBI testing in other parts of Canada and Australia has been shown to:
- Provide more privacy and reduce stigma
- Improve access in rural and underserved areas
- Allow people to test on their own time
- Increase acceptability of STBBI testing through providing alternative ways to test
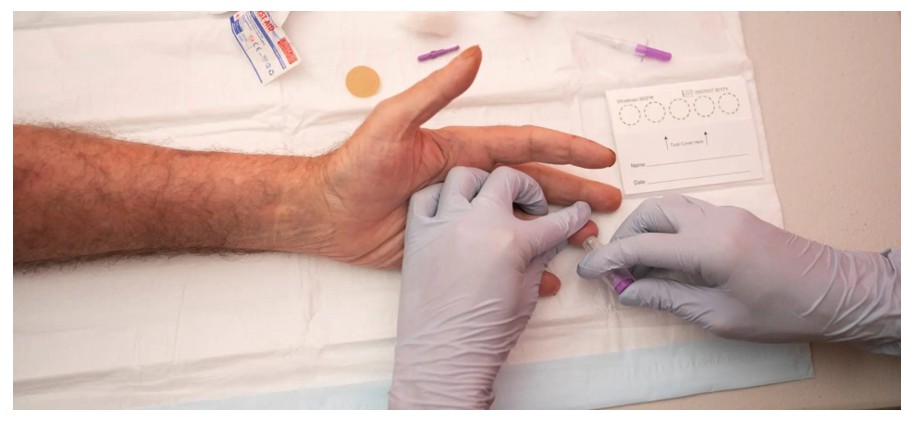 Figure 3. Example of dried blood spot (DBS) self-collection via finger-prick for STBBI testing. Available from: International Network on Health and Hepatitis in Substance Users.
Figure 3. Example of dried blood spot (DBS) self-collection via finger-prick for STBBI testing. Available from: International Network on Health and Hepatitis in Substance Users.
But testing is only the first step. It is also important to ensure that people can easily connect to care and treatment after testing. Further research is needed to understand gaps in access to STBBI care and treatment among people who access harm reduction services in British Columbia, and what types of strategies to address them will be acceptable.
Moving forward
This study is one of the first to examine STBBI testing uptake among people accessing harm reduction services across British Columbia. It highlights clear opportunities to improve access to STBBI testing by:
- Expanding testing within harm reduction settings
- Addressing gaps in rural and smaller communities
- Providing additional support for underserved health regions
- Improving awareness and understanding of test results
- Supporting community-led, peer-informed approaches

Figure 4. Shifting the narrative from hard to reach ‘groups’ to hard-to-reach services. Created by OpenAI and inspired by Juliet Young.
Ultimately, improving access to STBBI testing in harm reduction services will help reduce the public health impacts and burden on the healthcare system caused by these infections. This isn’t just a healthcare issue – it is also about equity, dignity, and meeting people where they are.
Learn more
Our study is published open access in BMC Infectious Diseases here and the full citation is:
Tiwana, A., Twohig, K. A., Fraser, M., Kinniburgh, B., Burmeister, C., Choisil, P., Haywood, E., Griffith, D., Xavier, C. G., Hannigan, A., Salters, K., & Bartlett, S. R. (2026). Sexually transmitted and bloodborne infections testing among people who use substances: Findings from the 2023 British Columbia Harm Reduction Client Survey. BMC Infectious Diseases. https://doi.org/10.1186/s12879-026-12924-4
