
 |
HIV and Housing |
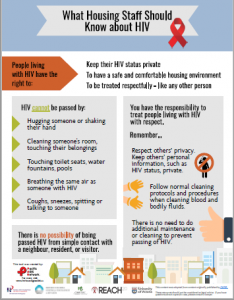
Click here to view/download a poster with information on HIV for housing staff.
HIV and Housing
As mentioned earlier, there are very few ways that HIV can be passed. In a housing situation, this means that there is no possibility of being passed HIV from simple contact with a neighbour, building resident, or visitors to housing.
HIV cannot be passed by:
- breathing in the same air as a person living with HIV.
- touching, repairing, or using belongings that may have belonged to a person living with HIV (for example, fixing a toilet or moving in furniture)
- talking to and spending time with someone.
Daily considerations
HIV is not passed through air. You can enter the home of a person living with HIV (for example, to help them move in, to bring them deliveries, or to visit) and breathe the air without any possibility of being passed HIV.
Touching the belongings of someone living with HIV, such as helping them move furniture or set up their apartment, has no possibility of passing HIV. You do not need to wear gloves or other protective clothing when touching, repairing, or using things that may have belonged to a person living with HIV.
You do not need to wear special protective clothing to do chores in the home of a person living with HIV, such as cleaning the bathroom, vacuuming, or washing the floors.
HIV is not passed through simple contact, such as shaking hands and hugging. When appropriate, you can engage in simple contact with people living with HIV without any possibility of being passed HIV.
Cleaning and maintenance
You do not need to do any special cleaning or maintenance in the homes of people living with HIV in doing routine tasks, such as cleaning floors or washing dishes. However, housing staff may have similar cleaning responsibilities to healthcare workers in terms of cleaning up blood and bodily fluids when necessary. The following information, adapted from resources from CATIE, will provide guidelines on cleaning up blood spills and bodily fluids. You may sometimes hear these guidelines referred to as “universal precautions” or “routine practices”. This poster from the Canadian Public Health Association, reprinted by CATIE, discusses universal precautions or routine practices in cleaning body fluids or fecal matter, and is available in both English and French: http://librarypdf.catie.ca/PDF/ATI-10000s/19661.pdf
Universal precautions/Routine practices
The Canadian Centre for Occupational Health and Safety (CCOHS) advises healthcare workers to:
- Act as though blood and all body fluids are potentially infectious.
- Report any needle-stick injuries to a supervisor or manager immediately.
For personal protection:
- Wear gloves when in contact with blood or other body fluids, excrement or non-intact skin.
- Wear gloves when in contact with articles such as clothing or surfaces that have been contaminated with blood or body fluids, and while cleaning or decontaminating an area.
- Replace torn or punctured gloves immediately.
Wearing protective eyewear, a mask or face shield and a gown during any procedure where droplets of blood or other body fluids may be produced is recommended.
Hand-washing is very important:
- before and after direct patient/client contact.
- immediately when there has been any contact with blood or other body fluid
- after removing gloves. It is important to know that our skin serves as a natural barrier. We wear gloves in case there is broken skin on our hands.
When cleaning up blood spills, the following steps will prevent the spread of blood-borne infections like hepatitis C:
- Wear gloves—torn gloves will not protect the hands from coming into contact with the blood.
- Carefully collect any sharp objects, such as broken glass, and put them in a sturdy plastic container such as one used for detergents.
- Wipe up the blood using paper towel or disposable rags and cloths.
- Disinfect the area with a solution of 1 part bleach to 9 parts water.
- Let sit for 10 minutes (at least).
- Wipe up the bleach solution using paper towel, disposable rags or cloths.
- Place the gloves, paper towel, rags and cloths into a durable bag and seal it.
- Wash hands thoroughly.
Disclosure and discrimination
As mentioned in the section of the Toolkit on personal information and disclosure, people living with HIV are not required to tell a landlord they are living with HIV, except in some special circumstances where this information is required to determine eligibility for housing.
Many people will choose not to mention their HIV status when dealing with housing matters. If you are aware of a building resident or neighbour’s HIV status, you should always keep in mind that this is private information. Sharing this information with others, such as residents and staff, could result in the person living with HIV experiencing negative impacts, including stigma and discrimination.
Moving out
You do not need to take any special precautions when a person living with HIV is moving out of their housing. No special cleaning (beyond what is necessary to make the space tidy, such as dusting, mopping floors, and other regular chores) or protective clothing is required when preparing the space for the next tenant.
HIV is not passed through air. You do not need to install any special air filtration systems to prepare the housing for the next tenant.
You can help someone living with HIV pack and move their belongings without any possibility of being passed HIV.
Key messages
The most important thing to understand is that there are very few ways that HIV can be passed, and that it is very difficult to pass HIV. You do not need to be concerned that you will be passed HIV through any common, daily activity. There are many ways to prevent HIV transmission, and HIV treatment can help to prevent HIV transmission in sexual contexts.
Contact information
For more on HIV, contact:
The Pacific AIDS Network, or visit the HIV Housing Toolkit at hivhousingtoolkit.ca
a public health unit
your local sexual health or family planning clinic
an HIV and sexual health hotline
your doctor or primary healthcare provider
a community health centre or, in Quebec, a CLSC
Resources:
Controlling Exposure: Protecting Workers from Infectious Disease, WorkSafeBC
Blood and Body Fluid Precautions, HealthLinkBC
This content was adapted from content originally published by CATIE, Canada’s source for HIV and hepatitis C information.
Routine practices and universal precautions (from Hepatitis C: An In-Depth Guide), CATIE
HIV Basics, CATIE
 |
 |
|
 |

